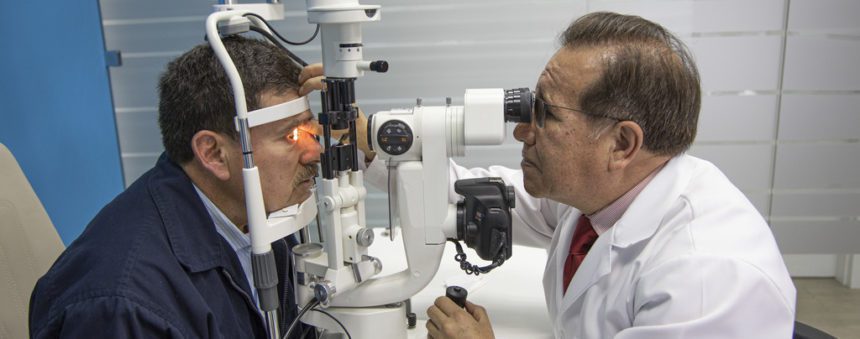
Radial interview to Dr. Christian Sancho, cornea and anterior segment specialist of Clinica Sancho, about eye care and eye symptomatology due to COVID 19.
How COVID can be transmitted to the eyes? What is the eye symptomatology and how is disease process?
What we have reported to this day according to the studies that have been presented, is transmission similar to conjunctivitis, which means that it is transmitted through the hands in many cases or by touching the eyes.
In turn, the issue of expectoration is another cause that apparently can cause conjunctivitis in the case of COVID. Regarding symptoms, there is conjunctival hyperemia (redness of the eye) similar to that of conjunctivitis.
What is the percentage of infection at the ophthalmological level?
According to reports, so far, about a third of the population sick with COVID, have conjunctivitis, but in the most serious cases.
What is the eye symptomatology?
What has been seen so far is that people have a red eye, what is striking is that it usually only occurs in one eye, there is no discharge as in other types of conjunctivitis. Apparently the behavior is a bit different.
It is a diffuse redness of the eye, patients also present a little photophobia, which means discomfort to light. That is the symptomatology that up to now we have been reported from Europe and China.
The area of the face and eyes are more vulnerable because people are used to touch or manipulate any object and then touch the face and eyes. What kind of hygienic measures should be taken?
This is why all decisions have been made at a global level about biosecurity that we must have, in this case, the health personnel who are treating this type of patients as well as the general population. This is based on how well it manifests itself in not touching our eyes, washing our hands permanently, the use of antibacterial gel with the appropriate concentration of alcohol, the use of protective glasses or face shields, in order to avoid any type of contamination.
The message here is hygiene, this is fundamental, the second is not to put your hands in your eyes and the third is depending on the conditions we are in, try to have glasses or easy protectors and finally, the permanent use of a mask.
Could the use of steam baths and sauna be an option to eliminate the virus?
It has no relationship, perhaps people think that high temperatures can eliminate the virus or that they will breathe better, but no, it is not like that, it does not serve us for these cases of coronavirus.
How to differentiate if I have conjunctivitis or I have been infected with COVID? Specially if there are not other symptoms.
In the specific case of conjunctivitis, it has variables. From what we have seen so far or from the reports that we have, it is that perhaps the differentiation that exists against common conjunctivitis is what I mentioned at the beginning; First, it is looked at if there is redness in the eye that may be diffuse (it means that it may be in several parts of the same eye but some areas are redder than others), it may present a little pain on movement, but it does not necessarily present discharge. Normally in conjunctivitis, one has a kind of discharge or mucus in great quantity, here it does not necessarily appear that way.
Now, if we do not have symptoms of the disease then, how can we detect if it is COVID? Well, through the tests that have to be carried out, that is, rapid tests, a swab; it is the only way to know if a person who is asymptomatic is infected.
What we can do if a child has red eye for several days?
In these cases we should determine several aspects: the age of the child, for example, allergic processes, but normally they should occur in both eyes, if it is only monocular, in only one eye, it is necessary to differentiate if there is pain, or not, if is that there is discharge or not, equally if there is a lot of tearing in the child or if it is simply redness. I think we should start from there and as a measure, what I would recommend is if obviously you do not have major discomfort and only the eye is a little red as it means that it is not an emergency, but nevertheless if this persists, one has to go immediately and seek ophthalmological help, currently there are several centers that we are providing care through telemedicine, without having to leave home.
In this quarantine all of us are spending a lot of time using computers, television and cellular phones. What recommendations you can give us to lubricate the eyes if people do not have drops or lubrication gel at home?
Indeed, the fact of exposing ourselves very often to all types of screens causes a certain type of affectation if their use is prolonged, we have to take into account that there are several types of screens where you have to start, one thing is the TV screen, Another thing is the screen of your cell phone and another is the screen of your computer. It will depend on what type of technology you have, normally today technology is based a lot on LED light and something that happens through LED light for example is that you have the toxicity of what we now call the famous “blue light”.
Many of the people will realize that in the cell phone, there is an option where it says “protection against blue light”, it is precisely one of the first things that one should activate on their mobile device or tablet, on the latest televisions generation usually already comes with that protection by default.
Logically, the longer we are exposed to this type of screen, the more irritations to the eyes are going to occur, however if one does not have the necessary tools such as an artificial tear, which is what is recommended in these cases since it can improve the situation, something that is also recommended is to rest a few minutes from the computer, apply what is known as an active pause, every 15 or 20 minutes to distract the gaze and blink for several times, you can also apply cold compresses that can be ice or ice cream on the eyes, close them for a moment and that will allow a lot of relief, something very practical is also to close your eyes and go to a sink and wash your face with plenty of water.
Swimming glasses can be used as protection to COVID -19?
To protect ourselves in these circumstances, it is not ideal since they can fog up, the patient may present discomfort, remember that this type of glasses uses a mechanism like a suction cup and I do not think it is the best way to protect ourselves.
What we can use to protect our eyes from COVID -19?
What can be done is to use a mask, gloves, use protective glasses, precisely to avoid contact with this type of virus, it is something that is being used globally.
If we have the means to disinfect the area where we are or when we are in contact with people who do not know where it comes from, then obviously alcohol, disinfectant or gel will be very useful.
What should I do to avoid the infection?
The most appropriate recommendation is to stay at home, however if you are going to go out, the recommendation is to take all the biosafety measures that we have mentioned, a mask, face shields or glasses, constant effective hand washing, according to the WHO recommendations. , gel or hand sanitizer with the appropriate concentration of alcohol and keep a distance of at least 2 meters between people.
When do you recommend that a patient with eye symptoms should visit your office?
If they are emergency cases, there are currently telemedicine options as a first resort, it is part of what has been handled, where certain patients and under certain conditions we can have an idea of ??how to guide them towards their diagnosis.
In very primary diagnoses, logically, go to the doctor if the discomfort is very persistent, if the eye, for example, is very red, there is a lot of pain, if there is suddenly a foreign body, in cases of accidents, progressive loss or loss of Sudden vision are emergency causes for which a patient should go to the consultation.